Health + Medicine
Feature
Osteoporosis and the Truth About Our Porous Bones
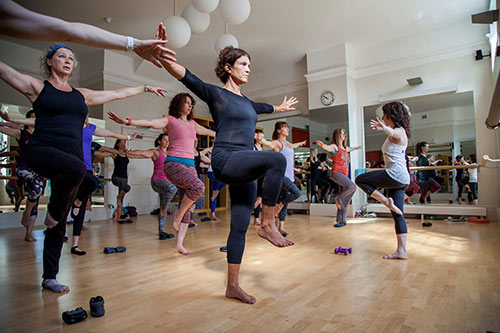
In 2004, Rebekah Rotstein listened to her doctor’s voice on the phone in shock. She had just been given the results of her bone density test and received a startling diagnosis. She had osteoporosis. In fact, her doctor told her that she had “the bones of an 80-year-old.” Rotstein was 28.
A former ballet dancer, Rotstein had worked in the sports medicine department in college and become a Pilates instructor. She describes herself as a lifelong “mover,” and so the news was devastating. “My body was my total identity,” said Rotstein, now a 42-year-old resident of New York City. “I felt like I was stripped of my right to free movement.”
Osteoporosis, meaning “porous bone,” is a disease in which bones lose their density and strength. The National Institutes of Health explain that healthy bones are made of living, growing tissue that under a microscope looks like a honeycomb. When the holes and spaces in the honeycomb become larger than normal, the structure begins to break down. When bone density is slightly low, it is called osteopenia. When it is more severe, osteoporosis.
Rotstein’s diagnosis was unusual since osteoporosis is most commonly found in postmenopausal women. According to the National Osteoporosis Foundation, about 80 percent of Americans with osteoporosis are women. Medical studies estimate that about one in two women and one in four men over age 50 will break a bone as a result of the disease.
Women make up the majority of those with osteoporosis because their generally smaller, thinner bones mean they have less bone mass than men. Another key factor is estrogen; the hormone’s level drops after menopause, causing bone loss that can increase the risk of osteoporosis.
Dr. Ethel S. Siris, director of the Toni Stabile Osteoporosis Center of Columbia University Medical Center, New York-Presbyterian Hospital, explained that there is a long list of medical and lifestyle issues that can impact bone density. These include taking steroids like cortisone and prednisone; drugs for breast cancer, such as aromatase inhibitors; overuse of stomach acid reducers like Nexium, Prevacid and Prilosec; and excessive caffeine or sodium consumption.
“Genetics is also a big part of it,” said Dr. Siris. “The size of your skeleton and the amount of bone that you build is largely genetically determined, also the quantity of bone that you lose after menopause. It’s often said that a mother with osteoporosis may well have a daughter with osteoporosis. But if your mother’s menopause was at age 40, she’s going to start losing bone at 40, which may be a good 10 years sooner than you would if your menopause was at 50.”
Different ethnic backgrounds carry different risks. According to the National Osteoporosis Foundation, Caucasian and Asian-American women are about twice as likely to develop osteoporosis as Latinas, and about four times more likely than African-American women.
Rotstein’s bone density test gave her a T-score, a measurement that compares bone density to the average in women around age 30. But a T-score does not represent a patient’s actual risk of fracturing a bone. Two women with the same T-score who are different ages with different lifestyles, health issues and other risk factors do not, in fact, have the same probability of falling and breaking a hip.
Some doctors have begun using an assessment tool called FRAX, which combines several clinical risk factors to calculate a patient’s 10-year risk of a hip or other major fracture. These include age, weight, family history, health issues and medications as well as smoking and alcohol consumption. Each patient’s situation is unique, and Dr. Siris stressed the importance of this when deciding to treat osteoporosis with medication. There is a range of drug options, including hormone replacement, which must be weighed against individual health risks; bisphosphonates, a class of drugs that includes Fosamax, Actonel, Boniva and Reclast; drugs that block bone loss like Evista and Prolia; and anabolic agents like Forteo and Tymlos, which help the body build more bone.
Bisphosphonates have been associated with serious health problems, such as osteonecrosis of the jaw, leading to bone pain and bone destruction. Dr. Siris said the risk is small and limited to patients taking high doses over several years. She maintained that taking appropriate doses with intermittent “holidays” from the medication is generally safe and can be very beneficial.
So, what would cause an active 28-year-old like Rotstein to develop osteoporosis? Rotstein found the answer in her adolescent and teenage years. According to the organization American Bone Health, children develop up to 90 percent of their lifetime bone mass by age 18. For girls, bone building is linked to the rise in estrogen when menstruation begins. If menstruation is delayed or stops due to high levels of exercise or extreme weight loss, girls can be at risk for poor bone development.
As a teenager, Rotstein was dancing intensively for eight years, and she was not menstruating for most of that time. Discovering the impact of this on her adult bones years later was “a wake-up call,” said Rotstein. To educate children about the risks to bone health, Rotstein has volunteered with the federal campaign Best Bones Forever!, which is aimed at kids aged 9 to 14.
Dr. Rivka Dresner-Pollak, head of the Department of Endocrinology and Metabolism at Hadassah-Hebrew University Medical Center at Ein Kerem, pointed out that eating disorders, smoking and alcohol can also affect bones.
“If we build stronger bones when we are young,” she said, “then we have a better reserve when we get older and start losing bone.”
New York City dietitian Keri Gans added that “a lot depends on your consumption of calcium and vitamin D and exercise as a youth.” Gans is concerned that many teenage girls begin to restrict their diets to lose weight, often cutting out milk and other dairy products.
The Recommended Daily Allowance is 1,300 mg of calcium for children aged 9 to 18; 1,000 mg for most adults but 1,200 mg for women over 51 and men over 71. Gans warns that while supplements can be useful in cases where calcium and vitamin D levels are low, they should not replace a balanced diet.
Rather than taking medication for osteoporosis, Rotstein was able to gain bone density through diet and exercise. Studies have shown that weight-bearing activities like walking, running and strength training can improve bone health even in elderly people. Doctors recommend avoiding specific movements like sit-ups or golf swings; and activities like skiing or ice skating, which can lead to falls.
In 2009, Rotstein developed Buff Bones, a research-driven exercise system for bone and joint health. Classes are available at locations across the United States and in 20 countries around the world as well as on the website buff-bones.com. The program draws on elements from Pilates, strength training, therapeutic exercise and functional movement patterns, to help strengthen bones and improve mobility and balance, Rotstein said, adding that the program is safe for osteoporosis patients.
One of Rotstein’s clients has been using exercise to manage her osteoporosis for the past six years. Renee, 69, a therapist and social worker who doesn’t want to use her full name to keep her health issues private, was diagnosed in her late 50s. She has been reluctant to use medication after finding herself sensitive to possible side effects from Reclast in the past. Renee has weekly sessions with a Pilates instructor and a physical therapist at her gym. “My doctor says I’m not in immediate danger now,” she said, “but I have to plan for the future.”
She believes she is already seeing the benefits. In 2010, she fell while crossing a crowded street and broke a hip, requiring surgery and rehabilitation. A year ago, Renee fell from a rock on a beach in Portugal and nothing was broken. “I’m attributing that to exercise,” she said. “Either that or good luck.”
Sarah Yahr Tucker is a writer based in Los Angeles, Calif.








 Facebook
Facebook Instagram
Instagram Twitter
Twitter

Ridley Fitzgerald says
It’s good to know more about osteoporosis. I like how you said that genetics is a big part of whether or not you get this disease. My family hasn’t really had this become a problem, so I’m hoping my kids will all be safe.
Beverly Roth says
My Dr. wants me to take PROLIA SQ every 6 mts. The copay is $640 but has side effects. Hve been on Fosamax & Ca Citrate. 5 am 84 with a diagnosed osteoporosis condition. What to the MDs think about a better diet and exercise?