Health + Medicine
Feature
In the Blood, Hadassah’s Bone Marrow Transplant Center
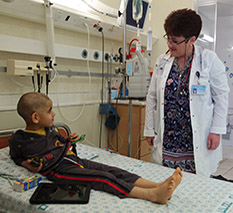
Dr. Polina Stepensky picks up her cellphone and clicks “Photos.”
“Look at my children!” she says in Russian-accented English. She brings up a picture of an 11-year-old girl wearing a Palestinian school uniform. The next image is of a sturdy blond Russian teenager in ice hockey gear. After him, the face of a 4-year-old fills the screen, mischief in his green eyes. Then there are two sisters, arm in arm. “They are from Tajikistan,” says
Dr. Stepensky. “We treated the older girl last year, and her sister is coming to us in a few months.”
By “my children,” it transpires, pediatric hematologist–oncologist Dr. Stepensky is talking about the dozens of youngsters whose lives she and her team save each year with bone marrow transplants at the Hadassah Medical Organization. “I feel like they are my own children,” she says. “We stay in touch, even though they are healthy and medication free.”
The impish 4-year-old, she says, was transplanted when he was 3 months old and does not remember her. But the teenage ice hockey player, who was suffering from a severe congenital blood disorder, was 9, and he and Dr. Stepensky formed a close connection.
“He is from St. Petersburg and spent a year in Israel for his therapy,” she says. “He is an only child, so there were no affected siblings. But many of the youngsters we treat are born to families who have lost one or more children to the same illness—inherited anemias, metabolic disorders and myeloproliferative diseases, along with blood malignancies such as leukemia, lymphomas and myelomas. Their parents have to watch them declining like the older children they have lost. With bone marrow transplant, we can often save them. One former patient is the only child in the world so far to survive his congenital disorder. Over 90 percent of the children we transplant are cured.”
With unflagging enthusiasm, Dr. Stepensky, 48, has headed the bone marrow transplant center at the Hadassah–Hebrew University Medical Center’s Department of Pediatric Hematology-Oncology for the past decade. Round-faced, warm and motherly, she is a medical high-flier. She built her department on the foundations of Israel’s first bone marrow transplant program, which opened at Hadassah 40 years ago, and rapidly brought her team to an international level in transplanting children with malignant diseases. It is, however, with bone marrow transplants in children with nonmalignant diseases, such as combined immunodeficiencies, osteopetrosis (genetic disease of the bones) and bone marrow failures, that she has broken new ground and made Hadassah a global referral center.
“Bone marrow transplantation is the only effective therapy for many disorders of the immune and hematopoietic systems,” Dr. Stepensky says. “Many of these diseases are inherited and, with high rates of inmarriage in many Israeli communities, we see a lot of them.”
Bone marrow transplant preparation differs for nonmalignant diseases, she says: “In leukemia, for example, the patient has usually been in chemotherapy, which has weakened the immune system. In a nonmalignant illness, the immune system, abnormal as it is, is nevertheless strong.”
Tasnim, the happy and healthy 11-year-old Palestinian schoolgirl pictured on Dr. Stepensky’s phone, was referred to Hadassah two years ago with constant respiratory infections, grave enough to hospitalize her. “When I met Tasnim, she was suffering a severe form of pneumonia,” says Dr. Stepensky. “Biopsy showed a serious problem in her immune system.”
Dr. Orly Elpeleg, head of HMO’s Genetic and Metabolic Diseases Department, was brought on board. She searched Tasnim’s genome for a coding-region mutation using a technology called Whole Exome Sequencing (WES). “Tasnim’s parents are first cousins and have many genes in common,” Dr. Elpeleg says. “That made it easier to recognize potentially harmful irregularities.”
Sure enough, a mutated gene (the IL-21 receptor deficiency), recessive in both parents, was dominant in Tasnim. It was responsible for her ongoing respiratory illnesses. “We searched the literature for other such cases and found four,” says Dr. Stepensky. “All had died. We were determined things would be different for Tasnim. We performed bone marrow transplantation, fine-tuning it with information from WES. We are the world’s only facility to use WES as a clinical as well as a research tool.”
With Dr. Elpeleg, Hadassah’s pediatric bone marrow transplant team has, thus far, found six genetic mutations linked to life-threatening disorders and is the first in the world to transplant and cure children carrying these genes. Most recently identified is a fatal blood disease known as TPP2 deficiency. “Our journey of discovery began a decade ago when a Palestinian toddler was brought to Hadassah Hospital with a severely malfunctioning immune system,” says Dr. Stepensky. “His 3-year-old sister had already died undiagnosed, with similar symptoms.”
Genetic sequencing of the family found a damaged gene that prevented correct expression of the TPP2 protein, resulting in premature aging of the immune system. Following a stem cell transplant in 2014, the child has been symptom free. The Hadassah team’s report of this case appeared in 2015 in Blood, the weekly journal of the American Society of Hematology. The article was named one of the journal’s top 10 stories of the year.
Performing up to 35 pediatric bone marrow transplants each year, Hadassah’s expertise is well known. With Dr. Stepensky a native Russian-speaker, many of her young patients come from the former Soviet Union, funded by Russia’s largest charity, Rusfond. Bone marrow transplants at Hadassah costs about $200,000—compared to $1 million in the United States.
Dr. Stepensky lays her achievements at the feet of her late father. “I am an only child, something common in Jewish families in the U.S.S.R. at the time,” she says. “I was born in Ukraine in 1967 in a town called Vinnytsia about four hours from Kiev. Like Kiev, it has a bloody Holocaust history. My father dearly wanted me to be a doctor, but ‘to be judged 100 percent,’ he used to tell me, ‘you have to achieve 200 percent, because we are Jewish.’”
Growing up, Dr. Stepensky strove for 200 percent. At age 19, she went to medical school in Ukraine. Four years later, halfway through her studies, she left for Israel. “I had married Igor, the greatest gift of my life, two years before,” she says. “It was 1990. Perestroika, [Mikhail] Gorbachev’s ‘reconstruction,’ was underway, and we grabbed our chance to leave for Israel. My parents followed a few months later.” They were among the hundreds of thousands of Jews who moved to Israel from the former Soviet Union in the 1990s.
The Stepenskys headed for Haifa. Igor, an engineer, found work with Israel’s merchant marines, which kept him at sea for six months at a time.
Dr. Stepensky enrolled in the University of Haifa’s Cheryl Spencer nursing school. “People said I had no chance of finishing my medical studies in Israel,” she says. With competition fierce for places in Israel’s five medical schools, without English and limited Hebrew, the advice was probably correct. Four years later, when Dr. Stepensky graduated as a registered nurse, she had upgraded her Hebrew, taught herself English and scored so high on the psychometric exam, Israel’s SAT equivalent, that she was offered a place at the Hadassah–Hebrew University School of Medicine.
Dr. Stepensky, her husband, their infant son, Yishai (born during her time in nursing school) along with Dr. Stepensky’s widowed mother, Rachel Bernstein, moved to Jerusalem. Igor quit the merchant marines, and eventually became chief electrical engineer in Israel’s Ministry of National Infrastructures, Energy and Water.
Bernstein looked after Yishai, and Dr. Stepensky plunged into her medical studies, paying her way through school as a pediatric nurse at Hadassah Hospital on Mount Scopus. “Hadassah gave me my chance,” she says. “They took me on as a nurse while I studied and credited me with three years’ medical school from Ukraine.”
With “giving 200 percent” ingrained since childhood, Dr. Stepensky made the dean and the rector’s lists. She also gave birth to a daughter, Yael.
Yael is now in her final year of high school. After her army stint, she plans to study psychology. Yishai has just completed his military service with the navy’s elite special operations unit, Shayetet 3.
Dr. Stepensky’s time as a nurse had a strong impact on her career, including helping her decide on a specialty—pediatrics. “My nursing background provided insights that do not come with a physician’s training,” she says. “It has given me enormous empathy for the parents of children I treat and a practical sense of what they can manage in caring for their child and, more important, what they cannot.”
Dr. Stepensky followed her pediatrics residency at Hadassah with a pediatric oncology fellowship under Dr. Yaacov Matzner, then-dean of Hadassah’s medical school, chairman of the Israel Society of Hematology and Transfusion Medicine and a global expert on blood diseases; he died in a plane crash in 2001. “He would say: ‘Our patients have been dealt so bad a hand that whatever we do will help them,’” recalls Dr. Stepensky.
Treating youngsters with blood cancers brought Dr. Stepensky to what would become her expertise: bone marrow transplants. To learn from the best, she spent 2008 as a visiting physician at the University of Minnesota Medical Center’s Blood and Marrow Transplant Program, the first place to successfully transplant human bone marrow between anyone other than identical twins. “I met giants of bone marrow transplant history there,” she says, “and I returned to Hadassah to practice what I learned—and to build a pediatric team that could give life to children facing death.”
While her work involves long hours, Dr. Stepensky’s zeal is undimmed. She has published over 60 papers and collaborates with research teams around the world. Last year, she was awarded prestigious European Union research grants—one for a trilateral and unlikely collaboration between Israeli, German and Palestinian researchers working on congenital diseases of the immune system.
Dr. Stepensky brims with plans. “I want to build an immunology lab at Hadassah’s medical school, and I already have some grant funding for this,” she says. “I want to develop our clinical work, train more people, do more.”
“Though,” she admits, wistfully, “it is impossible to do everything. I accept that.”









 Facebook
Facebook Instagram
Instagram Twitter
Twitter

Leave a Reply