Health + Medicine
Feature
Inside Israel’s Lifesaving Trauma Unit
Before this year, Israel and Poland inhabited different medical realities. “Poland hasn’t known war or terror, or experienced mass casualty, in a long time,”said Dr. Miklosh Bala, head of the trauma unit at Hadassah Hospital Ein Kerem. “They have no expertise in what Israelis face daily.”
Then, on February 24, Russia invaded Ukraine. Refugees streamed into Poland, and the risk of an errant missile or two slamming into a Polish civilian center near the country’s border with Ukraine became alarmingly real.
Just 11 days after the Russian invasion, Dr. Bala and his team flew to Poland with a Hadassah emergency medical delegation, the first of several Hadassah Medical Organization missions to the country. Part of the group went to treat refugees at a field hospital and refugee center in Przemysl, about 10 miles from the Polish-Ukrainian border. Dr. Bala, senior surgeon Dr. Asaf Kedar and Hadassah’s trauma nurse coordinator, Julie Benbenishty, went to the Medical University of Lublin. The city’s largest hospital, it had been appointed by the Polish government as a disaster center for the region.
“The hospital has excellent facilities and medical team, but no preparation for mass disaster or serious trauma events, and no systems in place for situations that challenge capacity,” said Dr. Bala. “We had a specific task: Teach local specialists the basics of disaster and mass casualty management.” Among the training and topics discussed were an introduction to disaster management, logistics around hospital preparedness and possible scenarios for mass casualty events. “We produced a training simulation and helped set up a real-time trauma guidance network with nearby hospitals.” While fears of a mass casualty event near Poland’s border with Ukraine have so far proven unfounded, Lublin’s hospital staff “was eager to learn, and we were proud to share,” Dr. Bala noted.

Born in the city of Grodno, now part of Belarus, Dr. Bala has shared his expertise around the globe, but it was in Israel where he first got his on-the-ground training. He made aliyah with a medical degree earned in Moscow and came to Hadassah as a resident in 2000, just as the second intifada began. Back then, Hadassah had Jerusalem’s only Level 1 trauma center, located at Ein Kerem. The first Level 1 trauma center in Israel, it had opened eight years earlier with support from Hadassah, the Women’s Zionist Organization of America. Today, the country has 21 trauma centers, six of them Level 1. Between 2000 and 2004, Hadassah treated half of the 8,341 people in Israel injured in the intifada.
Adi Hooja, then 11, was one of those trauma patients. She was severely wounded in April 2001, when a terrorist bomb packed with metal bolts blew up in the Jerusalem pedestrian mall where she had been getting an ice cream with friends. Dozens of metal shards perforated her leg. As the young girl lay near death in Hadassah’s trauma unit, the doctors made a difficult decision: They would not amputate. Multiple surgeries and long, intensive rehabilitation followed. Dr. Bala, now chair of the Israeli National Trauma Society, was a junior doctor on Hooja’s case. Today, the 32-year-old Hooja is married with children and walks steadily and gracefully.
In normal times—as normal as it gets in Israel—only 5 percent of HMO’s annual 2,500 trauma patients are victims of war or terror. “Trauma is physical injury that occurs suddenly—from road, work or sports accidents, falls and domestic or social violence, as well as from war and terror,” said Dr. Rami Mosheiff, head of Hadassah Ein Kerem’s orthopedic trauma department. Like Dr. Bala, he started working in trauma during the second intifada.

Typically involving complex and critical injuries that threaten life or limb, trauma care, or traumatology, is a multidisciplinary, multidimensional and constantly changing field. Trauma specialists must act fast and knowledgeably in the so-called “golden hour,” the 60 minutes after in jury when the right treatment reduces risk of death by a factor of three.
“Trauma care was once known as ‘the neglected disease of modern society,’” Dr. Mosheiff said. It was not identified as a separate discipline until the 1970s, he noted, though trauma injuries kill more people under the age of 40 worldwide than anything else, including cancer.
Israel’s lifesaving trauma protocols developed during the second intifada—from the number and specialties on the trauma team to the chain of decision-making—are globally recognized and shared at international conferences and in up to 20 academic papers a year. “It’s no overstatement to say we’ve changed the way trauma centers function,” said Dr. Bala. “Surgeons treating Boston marathon bombing victims in 2013, for example, used our triage methods and groundbreaking surgical procedures.” Among them was computer-guided technology, developed by Hadassah orthopedists for removing bullet fragments and repairing complex fractures.
Critical to Hadassah’s success in the trauma field are organization and teamwork, explained Dr. Bala. Organization is reflected in the defined chain of command, with the final call for a patient made only by a highly experienced trauma physician. Teamwork puts orthopedists, interventional radiologists, critical care staff, general surgeons and nurses on the trauma team.
The treatment of a family injured in a car accident in early May shows the system in operation. The father, who asked to remain anonymous, had lost control of his car outside Jerusalem as he drove his four children home from a wedding.The paramedics who arrived at the scene alerted Hadassah Ein Kerem’s trauma unit about the extent of the injuries as the ambulances raced to the medical center. Off-duty trauma staff hurried to the hospital to bolster its three on-duty physicians and two nurses, so that a full team of specialists awaited each patient. The children—aged 5, 8, 11 and 15—and their 46-year-old father were wheeled directly from the ambulances to the six-bed trauma unit, adjacent to Hadassah’s Judy and Sidney Swartz Center for Emergency Medicine. Each bed had a respirator, defibrillator and monitors as well as blood supply, antibiotics, pads, tubes, bandages and more. And each bed had enough space for multiple specialists to work simultaneously.
“Well within the golden hour, we’d assayed, X-rayed, scanned and assessed each patient, and started the treatment plan for each,” said Dr. Bala. “We treated all injuries successfully.”
Trauma care is a developing specialty, and today’s patients are more likely to be individuals or small groups, like the father and his children hurt in the car accident, rather than dozens or more victims of a catastrophe or attack. “The mass casualty situations of the intifada are now rare,” said Dr. Bala. A stark exception occurred on May 16, 2021, when three rows of bleachers collapsed in a Hasidic synagogue in northern Jerusalem on erev Shavuot. Two people died and 184 sustained severe crush injuries, head and abdominal trauma and broken bones. “We performed life-saving surgery—orthopedic, neurological and abdominal—all that night and the following day,” said Dr. Bala. Between Ein Kerem’s trauma unit and the regional trauma center at Hadassah Hospital Mount Scopus, some 150 people were treated, with the remainder going to other Jerusalem area hospitals.
Falls, especially among the elderly and, lately, severe injuries from electric scooter accidents, account for many of the trauma unit’s current patients. “With each new type of injury, we innovate, learn and craft more effective treatment techniques and protocols,” said Dr. Mosheiff.
Acts of terror that require trauma care are different these days, too. The second intifada’s blast injuries have given way to the crush injuries of car rammings and penetrating knife wounds. Dr. Bala recalled successfully treating a 20-year-old soldier, stabbed in the neck in Jerusalem’s Old City during the “knife intifada,” a wave of increased violence in 2015 and 2016. The soldier was taken to Hadassah Mount Scopus, and Dr. Bala and avascular surgeon were rushed thereby police car, with its lights flashing and siren blaring to get through the traffic, Dr. Bala said.
What has remained constant about trauma care are the miracle stories shared by specialists and surgeons. Dr. Mosheiff described an 11-year-old Bedouin goat herder who stumbled onto a mine in the Jordan Valley many years ago and was transferred to Hadassah Ein Kerem from a local hospital. “It had looked like we’d have to amputate both legs,” he said. “But, aiming to save not only his life but also his mobility, we decided to use one leg as a reservoir, drawing on its bone, vessels, ligaments and nerves to save the other. And the leg healed. Today, as an adult, he walks comfortably with a prosthesis.”
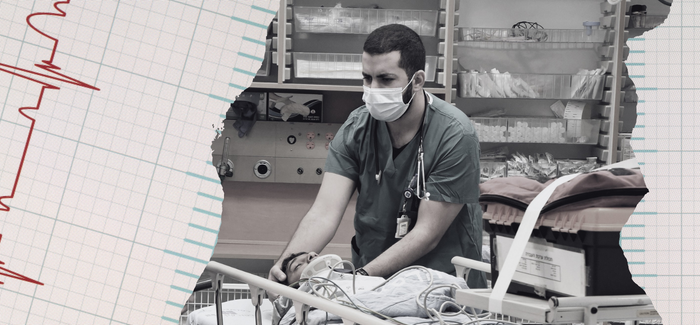
 A patient arrives at the trauma unit at Hadassah Hospital Ein Kerem.
A patient arrives at the trauma unit at Hadassah Hospital Ein Kerem.
For his part, Dr. Bala pointed to a 27-year-old woman who was in a driving accident a little over a month ago and brought to Hadassah Ein Kerem. “The paramedics judged her more shocked than hurt,” he said.“This was a rare occasion when they got it badly wrong.” Hadassah protocols require that all accident victims are first taken to the trauma unit, and it was there that trauma specialists discovered that she had sustained a life-threatening liver injury. “We treated her angiographically. Today’s technologies and better understand-ing of trauma physiology have made much trauma care far less invasive. Sometimes it’s better to keep your hands in your pocket than open the abdomen. Her recovery is slow, but she’s doing well.”
This young woman is one of 12 trauma patients currently hospitalized at HMO, all of whom are followed throughout their stay by the trauma unit team.
Traumatology, agree Drs. Balaand Mosheiff, is not for everyone. Its hours are disruptive, with surgeons and specialists called in for emergencies around the clock, and it requires vast physical and emotional stamina as well as theoretical and practical knowledge. Yet neither of the two specialists has ever doubted that the field was for them.
“I wanted this from the day I decided to be a surgeon,” said Dr. Bala, noting the satisfaction he gets from both directly aiding the severely injured and sharing his skills and knowledge with others. “It’s the best way I know to help people.”
Go behind the scenes at Hadassah Medical Organization with the Hadassah On Call: New Frontiers in Medicine podcast, hosted by Benyamin Cohen. This summer, episodes will highlight joint and knee care and diabetes research at Hadassah. Catch up on recent episodes, including an interview with Dr. Yoram Weiss, newly appointed director-general of HMO, who shares insights into emerging technologies and the future of medical care. Sign up for new episode alerts here.
Wendy Ellimanis a British-born science writer who has lived in Israel for more than four decades.









 Facebook
Facebook Instagram
Instagram Twitter
Twitter

Leave a Reply