Issue Archive
Medicine: Ready for Any Emergency
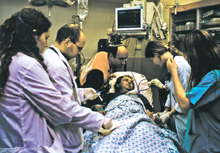
The fulfillment of a dream three years in the making, Hadassah’s new state-of-the-art Center for Emergency Medicine is spacious, bright and patient friendly.
For 12-year-old Benjamin, things grew steadily weirder. First there was the swelling in his leg, which grew so large and hurt so much his parents took him during the night to the emergency room at the Hadassah–Hebrew University Medical Center at Ein Kerem. Then in the morning, Ben was given a large teddy bear, loaded onto a gurney and amid smiling orderlies, nurses, doctors and his parents, wheeled out of the over-
crowded, outdated 30-year-old emergency room to become the first patient admitted to Hadassah’s new Judy and Sidney Swartz Center for Emergency Medicine (CEM).
It was Wednesday, December 22, 2004, less than three years since construction of the $50 million structure had begun. “This is a building in which to practice state-of-the-art emergency medicine,” says CEM head Dr. Jacob (Cobi) Assaf. “It’s a magnet to both patients and medical staff. It’s the fulfillment of a dream.”
While the new building comprises only two-thirds of what will be a 3,400-square yard emergency medicine center, it’s already double the department’s previous size and has twice as many beds. (It will take another year to integrate and convert the old ER to house the CEM’s main reception and triage areas; walk-in and minor-procedures clinics; and the X-ray; CT scan and ultrasound technologies of its imaging unit.)
“Until now, Hadassah’s was the only major emergency service in Israel that had neither been newly built nor undergone major renovation during the past five years,” says Dr. Shmuel Shapira, deputy head of the Hadassah Medical Organization. “And this was while we treated more than half of all Israel’s terror victims. Our ER’s record of care is excellent, but the facility was impossibly shabby and inconvenient, making it difficult both to work there and be treated there.”
The new center into which Ben was wheeled is bright and spacious, with cream-colored floors, teak-accented furnishings and recessed lighting. Its corridors, in happy contrast to the virtual obstacle course in the old ER, are wide enough for wheelchair and stretcher to pass one another with ease.
The gurney rolled Ben directly into the pediatric emergency unit, deliberately located next to the CEM’s main entrance to shield children from harrowing sights inside the main ER. It has a lounge and a play area and dalmatians that frolic on the tiled walls of its bathrooms. Of its 12 beds, two are for acute care and two are in private rooms for molested or abused children. The nurses station is at the unit’s center, all the beds around it.
“The radial arrangement was one of our basic principles,” says Dr. Assaf. “In each section of the CEM, the nurses stations are placed in the center so they can monitor every bed in every bay.”
A second fundamental was the division of the center into distinct areas. As well as pediatric emergency, it comprises an adult emergency unit (27 beds); a 12-bed trauma, resuscitation and critical care section (Hadassah is a nationally designated trauma center); and a 24-hour observation unit (12 beds). There are sections for triage; walk-in clinics (general, orthopedic, gynecological, psychiatric and ear, nose and throat); private rooms for highly distressed patients and their families (battered women, rape, accident and terror victims); family waiting areas; and its own imaging unit.
Basic principle number three was wide connecting corridors. Every part of the CEM opens onto at least one of three walkways that trisect it, which means patients and stretchers need never be wheeled through departments.
“As well as providing prompt and top-quality medical care,” says Dr. Assaf, “we aim to give patients high-level overall service. That includes making it easy for people to find their way around and get answers to questions, sufficient waiting rooms and rest rooms, kitchenettes, temperature control and wheelchair accessibility.”
These are the ideas that guided Hadassah’s multidisciplinary steering committee in designing the CEM. “We had a clear vision of what we needed, which we refined and developed with site visits to a dozen emergency rooms in Israel as well as to eight more in New York and Boston,” Dr. Assaf recounts.
While Hadassah has drawn on the experience of others, there are features of its CEM that are unique. First, Hadassah is simultaneously a community hospital, a tertiary referral center, a military hospital and a level-one trauma center. Its emergency patients thus present with a wide range of often severe and complex conditions, and the new center is designed to cope with all of them.
Second, with the harsh experience of the past four years in mind, its new CEM is designed for maximum flexibility: In time of mass casualty, its reception waiting area can be rapidly converted into an additional 10-bed treatment zone.
The new building is also proofed against conventional, biological and chemical attack. Its light, bright interior gives little sense of the massive exterior walls of reinforced concrete. Its thick windows and heavy steel outer doors are built according to Israel Defense Forces Home Command specifications, its air conditioning system is filtered and fire walls regularly space its corridors. A detoxification chamber equipped with high-power water jets and appropriate drainage will stand immediately outside its walls to decontaminate victims of chemical attack.
That, however, is not what is bringing about 200 patients a day to Hadassah’s CEM, a figure that has started to climb with the move.
“We always provided excellent emergency care, but it’s so much easier and pleasanter to do so in the new center,” says CEM head nurse Penina Sharon. “The place is still full and even with double the number of beds, we still have patients in the corridors, but there’s no feeling of crowding and tension any more. The whole atmosphere is so much more relaxed. I already have a stack of letters from discharged patients complimenting us on the care they received.”
The complex move to the CEM was meticulously planned. Monitors and call systems were checked, signs went up, mezuzot affixed, dust and debris cleaned and polished away, cupboards and drawers filled, beds made and walk-throughs taken to familiarize staff with everything from the floor plan to the location of bandages. It took a mere half-hour to transfer Ben and the other pediatric emergency patients. At that point, as if on schedule, an ambulance orderly called in to alert staff that a trauma patient was on the way. With all six of the new trauma beds primed and ready, the team had their choice for the teenage car-accident victim who arrived minutes later. Meanwhile, the relocation of adult emergency patients got under way, progressing as smoothly as that of the children. With most of the 27 beds soon filled, more than one staffer murmured, “However did we cope before?”
Every patient that day got a certificate declaring: “I was treated in the Center for Emergency Medicine on its first day.” Every adult was given a bag with toothbrush, toothpaste, soap, comb and a “Get Well Soon!” wish. Every child received a stuffed toy. For staff, too, there were souvenirs—pins with the slogan, Hai-Life: Every Second Counts—and it was not only emergency medicine staff who wore them. Physicians, nurses, paramedics, administrators, technicians, cleaners, pretty much everyone who works in the medical center found a minute to go across to the new CEM that day.
“In one sense, Hadassah remained Hadassah,” Sharon notes. “The patients were the usual mix of secular, Orthodox and ultra-Orthodox Jews and Arabs, young and old, presenting with fever, bleeding, pain, burns, shortness of breath—all the usual problems. But in another, it was completely new. The place is so beautiful, so well designed, so right for the needs it has to meet. It took my breath away!”
If the first day was one of joy and excitement, adjustment problems emerged during the weeks that followed. “It’s a new and much larger building, and we had to get used to that,” says Dr. Assaf. “The old ER was so small that people tended to shout from one side to the other, doctors read X-rays in its corridor and virtually everything and everyone was in view. Here, we have separate areas and use an intercom. The nurses stations function as nurses stations and we have a separate reception-cum-information center that fields phone calls and queries. That was a very big change.”
As well as the changes imposed by the physical space, Hadassah has taken advantage of the move to alter the CEM’s working system. “We’re now fully computerized from reception station to patient files,” says Dr. Assaf. He points to his mobile computer station. “I can wheel this to any patient and call up lab results or CT images within seconds of the procedure being performed. This allows faster diagnosis and definitive treatment, which helps ensure a steady patient-flow and reduces waiting time.”
“An emergency room is, for many patients, their first meeting with the medical center,” says Dr. Shapira. “It’s central to their view of both hospital and medical treatment. It’s their window on the hospital. I think that everyone involved in this building can take pride in the window they have created on the Hadassah Medical Center.”









 Facebook
Facebook Instagram
Instagram Twitter
Twitter

Leave a Reply