Issue Archive
Medicine: Re-creating the Womb
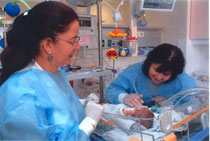
Hadassah’s refurbished neonatal unit cares for the smallest of premature babies, ensuring both the parents and child receive the support they need.
Were she not already a mother of three, Talya Cohn doubts she would have recognized as contractions the pains that began one afternoon, 26 weeks into her pregnancy. It never occurred to her to go to the hospital. Instead, she went to her own local doctor. The bleeding began while she was there.
“The doctor came with me in the ambulance to Hadassah,” says Cohn, who was then 29. “He told me I was in advanced labor, that I would shortly be having an emergency C-section and perhaps I’d like to call my husband.”
She remembers arriving at Hadassah, “feeling like I was in [the television show] ER, with faces above me, and a kind woman telling me she was a pediatrician and would be delivering my baby. I woke later to learn I’d had a boy and that he was on a respirator. I felt so ill, I did not ask to see him.”
Her husband, Chaim Cohn, had seen their son. That night, after putting their three older children to bed, he went to the Western Wall to pray for the baby—which he continued to do every night for the next three months.
“Elazar was born weighing a pound and a half,” says Talya Cohn, who had had placenta abruptio. “He looked like a little frog. His legs were no thicker than my fingers.”
That frail baby is now a sturdy 3-year-old. He is among 120 infants with birth weights less than 3 pounds who arrive in the world each year at both Hadassah Hospitals.
Despite the huge challenges facing these very premature infants, “their survival rate at Hadassah is 90 percent, with most having normal neurological development,” says Dr. Ilan Arad, head of neonatology at Hadassah. “This outcome equals that in leading medical centers in Europe and the United States.”
Since last summer, not only the statistics but also the new facilities at Hadassah’s Department of Neonatology have matched those of top hospitals worldwide. “Our department opened in 1977 and rapidly became a nationally recognized treatment center for critically ill newborn infants, but it also grew increasingly crowded,” says Dr. Arad. “Physically accommodating new techniques and knowledge about the human and psychosocial care of sick infants and their families was a growing struggle.”
The Department of Neonatology moved into the custom-designed 6th floor of Hadassah’s Mount Scopus hospital last July. The department’s original home, where the Cohns went daily for months to sit with their tiny son, had been essentially a corridor into the main pediatrics department. The new premises—10 years in the planning—are self-contained and double the previous size, giving each of neonatology’s three sections the space it needs.
The first section is a 30-crib nursery where full-term, healthy babies spend their first days of life—and are usually ready to go home before their exhausted mothers. Level 2 is an 11-crib (up from 8) intermediate-care nursery for babies who are sick or premature but not at serious risk. Level 3 is a 10-crib (up from 8) Neonatal Intensive Care Unit for infants born many weeks prematurely or with health problems so major (birth asphyxia, sepsis, congenital malformations, intrauterine growth retardation) that, until recently, they would not have survived at all.
“In the NICU, we’re essentially trying to re-create the womb,” says Keren Schaffer, neonatology’s head nurse.
Any successful duplication of nature’s incubator has been possible only since the 1960’s, when mechanical ventilation for newborns was developed, followed by a surge of new neonatal technologies.
In Hadassah’s refurbished department, many of these advances hang above each crib. From here, cardiovascular status is maintained, body temperature controlled, developing brains are checked, lung development aided and intravenous nourishment given until breast milk or formula can be tolerated.
“Maintaining the metabolic and physiological stability of these babies with their immature organ systems can have an important impact on both their survival and their future neurological development,” says Dr. Arad.
Technology is, of course, only part of re-creating the womb. The bonding between parents and baby is another key stress—which the department’s new home takes into full account.
“We virtually hospitalize the parents with the baby,” says Schaffer. “We give them practically unlimited access to their sick infants, even though working around them can be inconvenient. We use open incubators where possible, so they can touch and talk to their babies. If the baby’s skin is still too sensitive to be touched, we encourage parents to do the essential touching—diaper-changing, creaming, temperature-taking and so on.”
With more space available and the working conditions easier, the staff realized a long-term aim within weeks of moving. “Parents with babies in the NICU are usually distressed,” says Schaffer. “With our social worker, we have set up support groups of parents who meet, question, interact and compare experiences with a nurse there to give informed answers and allay doubts.”
Schaffer has also introduced a teaching course for parents. “Its main purpose is to give them confidence caring for babies who’ve had such a hard start,” she says. “We teach them general care, how to address life-threatening situations”—SIDS, food aspiration, electrocution, poisoning—“and train them in artificial resuscitation on a life-size doll. Our message is: ‘You’re your baby’s best doctor. You’ll know when something isn’t right, and you can always call us or come.’ Even our most senior doctors are available 24 hours a day.”
With family contact encouraged, certain restrictions must be in place. “Because most organ systems in preterm infants are immature, these infants are hypersensitive to light, noise and touch,” explains Schaffer. “Alarms in the unit are therefore visual, not audio, and lights dim.”
Along with hypersensitivity is the bugbear of all NICU’s: infection. “The underdeveloped immune systems of these infants makes infection control a major challenge,” says Dr. Arad.
The new unit is designed with this in mind. Cribs are widely spaced to reduce cross-infection. Every tiny patient has his or her own wastebasket, food heater and refrigerator in which to store breast milk or formula and medication. IV feeds are prepared in a closed room to reduce error. Medications are prepared in a second closed room, and all dosages are checked twice. The intermediate-care and NICU nurseries are even equipped for simple surgery, and there is a small laboratory for examining biochemical, hematological and blood-gas tests.
“We maintain a sterile environment throughout the NICU close to that of an OR,” says Schaffer. “We change ventilator suction tubes every day. With many of our babies hospitalized for weeks or months, we regularly change thermometers, ventilators and even their beds. No opened or half-used packets of anything are kept once a baby is discharged.”
One striking difference between the new facilities and equivalent departments abroad is the staff-to-patient ratio. Hadassah has only six full-time and one part-time senior neonatologist positions, only one nurse to every two to three babies in the NICU and one nurse to every five in intermediate care. All this in a department whose occupancy rate almost always exceeds 100 percent—all well below accepted norms in the United States. Despite this, according to Dr. Arad, it is the quality and devotion of the staff that give the department its prized reputation and a mortality rate lower than the national average.
“The nurse and doctors were truly wonderful,” says Talya Cohn of her experience. “They always had time for us and were always supportive.”
This level of commitment, however, comes at a price. “The work is physically, mentally and emotionally demanding,” says Schaffer. “Burnout among our nurses was very high until three years ago, when nurses were grouped into three teams, which rotate through the department every three months. This provides regular breaks from the intensity of the NICU, as well as a chance to see babies well enough to be discharged.”
The number of patients in hadassah’s newly housed department is expected to continue growing, but at a decreasing rate. “The number of low-birth weight babies is rising both because the population is growing and because new medical technologies save infants who once had no chance,” says Dr. Arad. “Both these trends can be expected to continue. But we can expect to see fewer babies [who have been] born too early because of reproductive technology and the multiple births in which it results.”
Reproductive technologies may be improving, reducing the number of multiple births and tiny babies, but triggers to extreme prematurity remain. Factors such as toxemia, high blood pressure, preeclampsia, infection, diabetes, kidney disease, hypothyroidism and placenta abruptio are among the known causes of 50 percent of early births. Add to this the number born with congenital disease and Hadassah’s renovated Department of Neonatology looks set to fill its little cribs for many years to come.








 Facebook
Facebook Instagram
Instagram Twitter
Twitter

Leave a Reply