Hadassah
Feature
Health + Medicine
Feature
BRCA, From Mutation Discovery to Survival

In Israel, some 4,500 women are diagnosed with breast cancer each year. The high rate of the disease—striking one in eight women, comparable to rates in the United States—ranks Israel among the world’s most afflicted countries and gives Dr. Tamar Yablonski Peretz what she calls “the unique vantage of probably treating more Ashkenazic Jewish breast cancer patients than any other physician anywhere.”
Dr. Peretz heads the Hadassah–Hebrew University Sharett Institute of Oncology in Jerusalem and directs its Center for Malignant Breast Diseases. She was part of the international team that, in 1994, showed the cancer-linked BRCA gene mutation is 10 times more frequent among Ashkenazic Jewish women than in the general female population. “It’s important to identify the mutation not only for prevention and early detection, but also for therapy,” she says. “The disease must be treated differently in those who carry it—generally with aggressive chemotherapy, a different surgical approach and tailored biological therapy.”
According to the Israel Cancer Association, there were 21,155 breast cancer survivors and newly diagnosed breast cancer patients between 2008 and 2012. Hadassah, with its multidisciplinary, personalized approach to the disease, is developing therapies and reaching out to new communities for research and treatment.
While there is overall consensus on therapy among breast cancer experts worldwide, where views clash is whether all Ashkenazic Jewish women should be routinely screened for the three BRCA mutations that increase the lifetime risk of breast and ovarian cancer by up to 83 percent. For many, this is a no-brainer: Mary-Claire King, Ph.D., professor of genetics at the University of Washington School of Medicine, whose lab provided the first evidence of the mutation in 1990, is quoted in a 2014 JAMA publication saying: “To identify a woman as a carrier only after she develops cancer is a failure of cancer prevention. All women over age 30 should be tested for the gene.”
But Dr. Peretz strongly disagrees. She opposes universal testing for BRCA mutations as well as universal testing of Ashkenazic women. “Informed decisions about the impact of testing are often overlooked,” Dr. Peretz says. “Testing must go together with genetic counseling, which includes evaluation of the patient’s emotional status, preferences and family history. Testing alone doesn’t give a sufficiently complete picture for complex and life-altering decisions about preventive surgery, possible infertility and early menopause.”
Nor does a BRCA mutation solely affect the patient, she says. Each first-degree relative has a 50-percent chance of carrying that mutation. The patient must decide whether and how to tell them. So screening must be part of oncogenetic counseling in which the consequences to the woman and her family are addressed.
Of Israel’s BRCA mutation carriers who show no signs of cancer, only 15 percent opt for preventive double mastectomy. Dr. Peretz is comfortable with this. Close monitoring is, she says, “an acceptable alternative. At Hadassah, we have a dedicated clinic for this high-risk population and are well placed to identify the disease at its earliest and most treatable stage.”
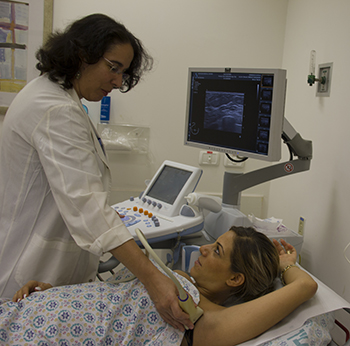
Hadassah’s high-risk clinic is a “one-stop shop for BRCA-mutation carriers from age 25,” says Dr. Luna Kadouri, a senior physician and genetic oncologist at the Sharett Institute. “They come to us twice a year for MRI mammography and breast and uterine ultrasound. They consult with the clinic’s oncologists, radiologists and gynecologists, fertility counselors, psychologists and social workers—and, when necessary, with its surgeons.”
Dr. Kadouri has been active in genetic counseling and risk assessment in breast and ovarian cancer since the Clinic for Oncogenetic Counseling opened in 1995 in the Sharett Institute. She also works for the Center for Malignant Breast Diseases’ Risk Evaluation Program, counseling patients together with a medical oncologist. “In the general population,” she says, “we test for dozens of cancer genes, but in Jewish patients we begin by checking for the mutations we know are common among them.” With Dr. Peretz and collaborators from Hadassah’s Department of Genetics and Metabolic Diseases, she has found BRCA mutations specific to Jews of Yemenite and Kurdish origin. The team is currently investigating BRCA in Israel’s North African Jewish and Palestinian populations.
“We all express BRCA in breast and other tissue cells—and still call it BRCA [BReast CAncer gene], even though we now know it’s linked with ovarian, colon, pancreatic and prostate cancers,” says Dr. Kadouri. “Part of its job is coding for proteins to repair damaged DNA. When BRCA is itself faulty, it can’t do a proper repair, increasing risk of cancer.”
Israel’s high rate of BRCA mutations has attracted international pharmaceutical companies seeking to prevent or mend the damage wrought by the faulty gene. One promising approach is PARP inhibitors that block an enzyme in cancer cells. Clinical trials of this new type of targeted therapy are underway at Hadassah.
Although breast cancer kills some 900 people in Israel each year, survival rates are increasing. The International Agency for Research on Cancer ranks Israel fifth highest in incidence of breast cancer, but only ninth (and declining) in mortality.
This is largely explained by the increase in early detection. Outreach to heighten awareness of breast exams began in the mid-1990s with immigrants from the former Soviet Union. It now extends to other communities as well, especially those neglectful of breast health.

“I remember talking to newly arrived Ethiopian women and showing them how to self-examine—most with a baby tied to their backs,” says Ilana Kadmon, Ph.D., Israel’s first clinical breast-care nurse specialist and today a senior faculty member at the Henrietta Szold Hadassah–Hebrew University Nursing School. The proportion of Arab women undergoing biennial mammography—covered by Israel’s health care system for women over 50—has risen from 49 percent in 2001 to 70 percent today. Hadassah also has targeted ultra-Orthodox women, where outreach coordinators made an unexpected finding: Incidence of breast cancer is lower among haredim than in the general community, but patients present at a younger age and a more advanced stage.
Israel’s multiethnic society propels Hadassah Medical Organization’s genetic oncology approach, which tailors therapy to individual patients according to genetic profile. This emphasis on the individual meshes with the way HMO supports breast cancer patients. The five-year-old Marlene Greenebaum Multidisciplinary Diagnostic Breast Center at Hadassah–Hebrew University Hospital at Ein Kerem is a single, rapid access point to biopsy, ultrasound, radiation, consultation, treatment and follow-up. “In breast cancer, there are a lot of difficult moments and a lot of hope,” says radiation oncologist Dr. Tamar Sella, head of the Greenebaum center.
Support also comes in the form of a clinical nurse specialist in breast care. Kadmon pioneered the specialty in 1994 at Hadassah Hospital, with the support of the Israel Cancer Association. Today, there are 40 specialists nationwide. “The job is to meet every woman with breast problems and help her navigate the system,” says Kadmon, whose Ph.D. is in breast cancer’s psychosocial effects. The nurse specialist “sees to referrals, helps in decision making and gives psychological support.”
HMO introduced not only the breast-care nurse specialist to Israel, but also the discipline of psycho-oncology. Lea Baider, Ph.D., joined the Sharett Institute in 1979 as a senior psychologist and within a decade set up a dedicated Psycho-Oncology Unit. Today, at the age of 76, the Hebrew University professor emerita of psychology volunteers in the unit.
“The level of psychological distress and ability to adjust to a diagnosis of cancer are highly variable,” she says. In addition to treating thousands over the years, Baider has examined how cancer patients cope with the trajectory of their illness as well as the influence of gender, marital status and spiritual beliefs in families struck by cancer. She has carried out groundbreaking research—“the most focused and comprehensive ever to be conducted in the field,” says Dr. Peretz—into the response of Holocaust survivors and their families to a breast cancer diagnosis.
“This population has unique concerns and needs,” says Baider. “We’ve found they experience especially high levels of anxiety and depression and, unlike other patients who generally benefit from group therapy, find it hard to talk about a cancer diagnosis in a group setting. They need one-on-one emotional support.”
This heightened reaction to breast cancer also occurs in the daughters of survivors. “Vulnerability in a traumatized generation is passed down,” Baider notes. “Middle-aged women with breast cancer born to Holocaust survivors experience far greater depression, anxiety, hostility, obsessive thoughts and psychosomatic symptoms than average. Women with living survivor mothers suffer the most severe symptoms. I believe that, in a decade or so, oncologists will see similar reactions among third-generation Holocaust survivors.”
“Breast cancer is no longer an automatic death sentence,” notes Dr. Peretz, “but it remains a serious illness.” Today, newly diagnosed patients and those carrying the mutated gene face a bewildering array of treatment options and opinions. This will change, she adds. “Treatment will become increasingly personalized—structured according to the many factors involved, from genetic to emotional. Decisions will be easier and results will be better.”








 Facebook
Facebook Instagram
Instagram Twitter
Twitter

Ellen Levine says
I’m making Aliyah to Jerusalem. I had ILC 6 years ago and am in remission.
My recent genetic testing revealed the CDH1 mutation. I’m having an endoscopy with biopsies tomorrow.
Who at Hadassah treats patients with this mutation and HDGC?
I am a patient at Beth Israel Deaconess MC in Boston and I want to know if Hadassah can offer me an equivalent level of medical expertise. My oncologists at bidmc are Nadine Tung and Katherine Germansky.
Thank you