Health + Medicine
Feature
Lessons in the Pediatric Wards

It took 7-year-old Malik only moments to decide that “Despacito” is his favorite song. An Arabic version of the Puerto Rican pop hit was found on an iPad, and he and other youngsters accompanied its Latin rhythms on drums, cabasas, maracas and cymbals.
Moishy was next. The 4-year-old’s choice was a world away. Clutching a silky earlock, the shy youngster whispered in Yiddish to his father, and the beat segued to a Hasidic tune praising kabbalist sage Shimon Bar Yochai.
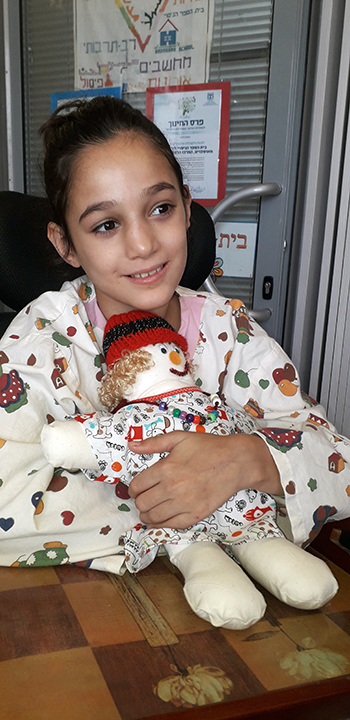
And 11-year-old Yuval Itskovitch, wheelchair-bound after a road accident shattered her pelvis, hesitated to name her favorite, a Hebrew song about a mother grieving for her soldier-son’s death. “It’s a really, really sad song,” the slender preteen said softly.
“That’s O.K.,” responded music teacher Sivana Dardik. “Everyone here has known sad moments.”
“Here” was a music class in the kitchenette of Hadassah Medical Center’s pediatric surgery department in Ein Kerem. The class is part of the Hadassah School, which educates through informal learning and one-on-one tutoring the several hundred pediatric patients hospitalized at Hadassah’s two Jerusalem campuses.
The weekly music class—like others in the school—is open to all patients aged 3 to 21, and many come with their parents. This one was well attended: More than a dozen children sat in front of their parents around the kitchenette table as dishes from an earlier cooking lesson (which tempted dulled appetites while teaching weights and measures) were drying near two large sinks. The windows of the room overlooked the Judean Hills. A glass wall separated the space from the department’s busy family lounge.
“Tell us your name and choose an instrument,” urged Dardik, with colleague Mira Elayyan translating into Arabic (and Moishy’s father rendering what Dardik said into Yiddish). One child selected a stringed gourd, another a darbuka drum. There were constant interruptions—16-year-old Ahmad was called for therapy; another child arrived late—yet the group gelled. Names were repeated, youngsters were encouraged to interact, and somehow these seriously ill children from widely different backgrounds began relating to one another.
“Malik is so sweet,” said Yuval, who lives in Tzur Hadassah, about seven miles southwest of Jerusalem. “I see he’s sick, but he’s so full of life, so mischievous. He makes me smile!” Ahmad’s mother, Fatima, who, like many of the parents interviewed declined to give her child’s full name or the details of his illness, told Elayyan: “This music group is a highlight for Ahmad. It’s the most normal thing he does at Hadassah.”
Israel is one of the few countries around the world where some sort of daily schooling for long-term pediatric patients up to age 21 is compulsory. Sunday to Thursday, Hadassah School teachers, all with Ministry of Education accreditation, visit children admitted to Hadassah’s 10 pediatric departments. They determine who is up to attending the school’s informal classes on cooking, art, music and nature, and who requires bedside learning. Academic subjects such as math, writing and history are taught as well, largely through tailored one-on-one instruction. Hadassah teachers help children keep up with their regular classwork, too, usually using material sent by the patient’s own school.
From the outset, the Hadassah School has been a pioneer among individualized study programs and nontraditional education initiatives, thanks to longtime principal Edna Pinchover, a diminutive, energetic 64-year-old from Hadera.

“I used to be sent the ‘difficult’ children, and found I was good with them,” Pinchover said, recalling her time as an art instructor before she came to Hadassah. “That got me thinking. Children are difficult when they have problems. Sick children have many problems. So I dared to dream about teaching children in
a hospital.”
She soon discovered that there were no learning programs for children in Israel’s hospitals. “Hadassah once had a games center, so I started there,” she said. “It took me a year to convince the head nurse. When she finally hired me, it was in a nurse’s job slot.”
That was 1983. The following year, Israel’s Ministry of Education, which oversees both formal and informal education in the country, recognized Hadassah’s school and officially appointed Pinchover as principal. Three years later, the school hired a second teacher. Today, it has 80 educators, many of whom have a background in special education, and 20 volunteers, all of whom coordinate with doctors, nurses, therapists, social workers and others to provide patients with schooling. In 2014, the school, which is financed by the Ministry of Education, received the National Education Award, the Israeli government’s highest award for an educational institution.
To create the complex educational setting that became Israel’s first hospital school, Pinchover found herself building a unique curriculum, a blending of formal individualized education and informal classes that speak to the young patients’ experiences. “Our pupils are bewildered by their physical and emotional circumstances, cut off from the familiar, coping with a challenging medical world,” she said. “Our school reminds them that they’re not only patients but also students capable of learning.”
Zaynab, for example, should have started first grade in September, but instead found herself a pediatric oncology patient. Like her healthy peers, however, she spends an hour or two each day learning to read and write with the help of a teacher who either visits her room or sits with her in one of the hospital lounges.
Shani, a bright and motivated 14-year-old hospitalized for her 31st surgery, is in eighth grade. She is preparing for high school but has been in and out of the hospital, with at least a dozen more surgeries scheduled to replace the black-pigmented skin that covered 70 percent of her body at birth. “Hadassah helps her keep up” with her peers, said her mother, Meshi.
Yuval, now finishing elementary school, is worried about transitioning to junior high. She has missed midyear exams in English and Bible, which could affect her placement next year. In pain and unable to concentrate for long, she may be a candidate for a remote-learning pilot program that digitally connects students with their classes, sustaining both studies and friendships.
 “Helping children keep up with the national curriculum is part of a hospital school’s responsibility,” said Rim Alyan, who has taught at Hadassah for 12 years. “Another important part, however, is being relevant to the children we teach. Their lives are about the hospital, therapy, illness and pain, blood tests, angiograms, scans and surgery. They’re constantly required to do things they don’t understand, and this often frightens them. Understanding what’s happening makes a huge difference.”
“Helping children keep up with the national curriculum is part of a hospital school’s responsibility,” said Rim Alyan, who has taught at Hadassah for 12 years. “Another important part, however, is being relevant to the children we teach. Their lives are about the hospital, therapy, illness and pain, blood tests, angiograms, scans and surgery. They’re constantly required to do things they don’t understand, and this often frightens them. Understanding what’s happening makes a huge difference.”
She recalled a quiet 9-year-old who required bedside instruction because of a temporary postsurgical drain in her neck. Alyan, visiting daily, gained her trust. “Too afraid to ask her doctors and nurses,” Alyan said, “she nervously asked me: ‘Is this thing going to be in my neck forever?’ ”
Understanding hospital procedures—from surgical drains to blood tests—is the purpose of the Hadassah School’s MEDucation program. Offered as needed, depending on the patient population, the program’s blood-test kit, for example, includes a syringe, gloves, red-colored water and a rolled bandage that youngsters jab to find a “vein.”
“We tell them: ‘There are two-and-a-half Coca-Cola bottles of blood in your body, and the syringe holds less than a teaspoon,’ ” said Pinchover. “We explain why gloves are used, and what the doctor sees in their blood—that is, basic biology and some math—and encourage youngsters to share with one another.”
The program has not only increased the children’s compliance with medical procedures, it has also helped some of these young patients lighten what can be a heavy pharmaceutical load.
“Because patients in radiotherapy must remain immobile, children who have difficulty being still are sedated,” explained Pinchover. “This can mean daily sedation and fasting. We built a fake linear accelerator”—a radiotherapy machine that targets the region of a tumor—“equipped it with a real bed and a life-size doll, and used it to teach young patients to keep still during the therapy.”
Seven-year-old Yitzchok is a MEDucation success story. “I lie perfectly still each time for 20 whole minutes!” boasted the young boy. He was receiving daily radiation for malignant tumors in his chest and stomach, and now no longer requires sedation. “The school made me a party for lying still!”
All the children in the pediatric oncology department were invited to Yitzchok’s party. Like other school classes and events, it was designed to help the young patients connect in an environment where it is generally hard to find same-age peers or friends. Some exceptions do exist. Two little boys, both Palestinian, made a beeline for one another in the music class. Shani relies heavily on Ruthie for emotional support; both were born in Hadassah on the same day and both are disfigured by giant nevi. Their multiple skin-graft surgeries are scheduled to take place at the same time. An intense friendship developed between two 15-year-olds with cancer—one from Russia, the other a Bethlehem native.
For these hospitalized youngsters, peer pressure is replaced by the challenge of diversity. Classmates are different ages, speak different languages and come from different cultures, ethnicities and faiths.
The same is true of the teachers: Like their pupils, they are haredi, traditional and secular, Jewish, Muslim and Christian, Israeli and Palestinian.
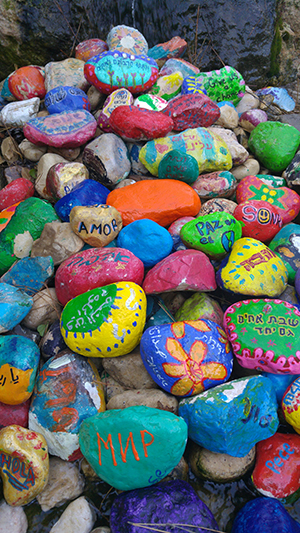
“Their unexpected encounter with ‘the other’ can be shocking,” said Pinchover. “More than one Jewish family has objected to an Arab doctor or nurse treating their child. More than one Muslim youth has loudly bragged about throwing stones at Jewish Israelis.”
Instead of warily stepping around the divisions, which is what the school used to do, said Pinchover, 12 years ago, the program decided to “embrace multiculturalism formally and make conflict resolution part of our curriculum.”
Tensions are creatively addressed through talk therapy, art projects and one-on-one encounters. Rocks, for example, an emotive symbol of the Israeli-Palestinian conflict, were the center of a school peace project in 2016, with children painting their hopes for peace onto stones. A photo of a child holding her stone was taken by Mohammed Abdeen, then an 18-year-old Hadassah pediatric patient who won a photography contest sponsored by the United States Agency for International Development’s Office of American Schools and Hospitals Abroad. That stone as well as the others created by patients are now in the Healing and Environmental Garden of Hadassah’s Center for Children with Chronic Diseases.
“Hospitalization is a rare opportunity to break down stereotypes and prejudices,” said Pinchover. “We work to ensure our pupils have a positive multicultural experience here that neither they nor their families will forget.”
The final word on Hadassah’s school, however, belongs to its pupils. Yuval said that she initially was not enthusiastic about attending the classes. Yet she found herself “really enjoying being with other kids, learning things in a new way, understanding more of what’s happening to me and,” she added, “best of all, being ‘Yuval’ and not ‘the girl who broke her pelvis in a car crash.’”
Wendy Elliman is a British-born science writer who has lived in Israel for more than four decades.








 Facebook
Facebook Instagram
Instagram Twitter
Twitter

[…] Lessons in the Pediatric Wards […]