Health + Medicine
Feature
Call the (Hadassah) Midwife
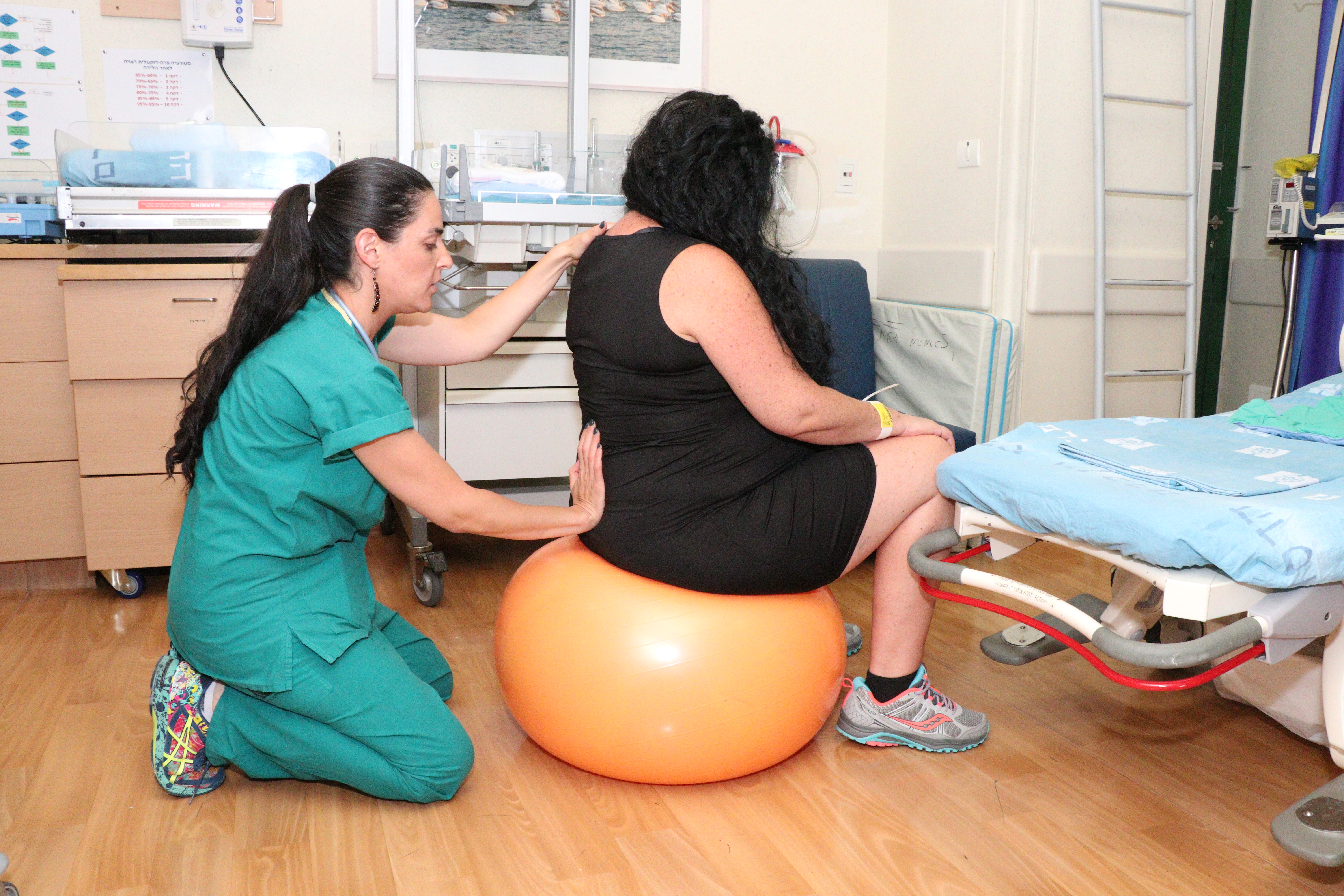
It was Liya’s sixth baby. her others had been born in Ethiopia, her mother’s strong, gentle hands stroking her belly as sunlight filtered through the thatched roof and mud-plastered walls of her home. Liya, who moved to Israel with her family in 2017 and preferred not to give her last name, gave birth to her youngest child in the delivery room of the Hadassah-Hebrew University Medical Center in Ein Kerem, monitors beeping in the background.
“Her labor had stalled, and the obstetrician wanted to start her on Pitocin,” said Hadassah midwife Batya Kaplan. “I asked him for a few minutes because I sensed this wasn’t how she wanted to birth her baby.”
The obstetrician-gynecologist readily agreed, and Kaplan cleared the room of nonessential personnel. She grouped the medical students out of Liya’s line of sight, dimmed the lights and flattened the birthing bed to resemble the stone pallet where Liya’s other babies were born. “She relaxed,” Kaplan said, “and very soon a healthy little girl crowned, without medical intervention.”
Kaplan is one of nearly 90 midwives at the Ein Kerem hospital. This year—designated by the World Health Organization as the Year of the Nurse and the Midwife—they will collectively attend nearly 8,000 births. Another 5,000 babies will be born at Hadassah’s Mount Scopus campus, attended by its own midwife team in their newly renovated maternity suites.
“Our emphasis is helping every woman give birth safely in the way she wants, whether that’s natural childbirth, an epidural or anything in between,” said Nava Braverman, head midwife at the Ein Kerem hospital. “Childbirth is among the most important events in a woman’s life, and it’s our job to ensure the experience is good and safe for her and her baby.”
Ariella Kaplan (no relation to Batya) delivered her first two children in Boston, where she and her husband, Yotam, temporarily moved while he studied for his Ph.D. at Harvard Law School. Their son, Daniel, now 7, weighed in at 9 pounds and was delivered by C-section after a 27-hour labor. Keren’s birth, three years later, was a repeat, though labor was far shorter before the doctors went ahead with a C-section.
“With my third, I wasn’t going through surgery again,” said Kaplan, who opted not to have an epidural. She said that her Hadassah ob-gyn, Dr. Matan Elami-Suzin, confirmed she was a good candidate for VBAC, vaginal birth after Cesarean section. Talia was born vaginally, following 15 hours of labor. “Dr. Elami-Suzin and the team were amazing. There was such warmth among them. When I felt I couldn’t go on, my midwife, Yanna [Glazer], focused me, helped me breathe and push. Two hours after giving birth, I was standing in the shower.”
As experts in pregnancy and birth, midwives—the word derives from Old English mid (with) and wif (woman)—have earned a respected place in Israel’s birth culture. Their profession goes back at least to ancient Egypt, where the biblical Shifra and Puah displayed characteristic midwife spirit in defying Pharaoh’s command to kill newborn Hebrew boys. For second-century Greek physician Soranus of Ephesus, a midwife had to be “literate, with her wits about her, possessed of a good memory, loving work, respectable and…endowed with long slim fingers and short nails at her fingertips,” as he wrote in his treatise on gynecology.
Listen to The Branch episode ‘The Midwives’ with Hadassah midwives Gila Zarbiv, a Jewish Israeli, and Rahel Najwan Rasslan, an Arab Israeli. Amid a surge in the coronavirus in Israel, the two work side by side at Hadassah Hospital at Ein Kerem to calm mothers bringing new life into an uncertain world.
In prestate Israel, as elsewhere until early last century, midwifery required no qualifications. It took until the 1980s for midwives in Israel to become the trained obstetrics professionals of today. All Israeli midwifes are required to complete a four-year bachelor of science in nursing, at least a year working as a nurse, a one-year midwifery specialization and two to three years of on-the-job experience. (In the United States, midwife accreditation does not require a nursing degree, and the closest equivalent to Israel is a nurse-midwife.)
Danya Meirovich said she was attracted to midwifery by “the independence of midwives and their quick decision-making that profoundly impacts the women in their care.” She said that in her 15 years at Hadassah, “I’ve fallen in love with working with women. Every woman is different, every birth is different. We must read each woman, understand her expectations, needs and fears, and empower her during the powerful experience of birthing.”
In 2018, with midwifery-attended pregnancies around the world linked to fewer epidurals, episiotomies and instrumental births as well as lower risk of early miscarriage, the WHO formally recommended midwife support of women throughout normal pregnancy, labor, birth and follow-up.

Unlike in the United States, where midwives are often seen as an alternative option in the birth experience, Israeli midwives routinely fulfill the WHO’s labor and birth recommendations. They are involved in delivering the majority of babies in Israel and work mainly in hospital settings. However, midwife involvement in prenatal and postpartum care as well as private practice, according to Braverman, is still “a dream in the context of Israel’s current health system.”
At Hadassah, midwives are active in the labor wards, delivery rooms, prenatal high-risk clinics and operating rooms. Thanks to them, many natural birthing protocols, including skin-to-skin contact between mother and baby immediately after delivery and delayed umbilical cord clamping, are now emphasized. Hadassah’s midwives are also known for creative programs and thinking on their feet, which became paramount in recent months as pregnant women with Covid-19 have gone into labor.
The first such mother-to-be in Israel was brought to Hadassah on March 16, and, writing their own protocol, Hadassah midwives and doctors designated an isolated room with one midwife next to the laboring woman and another outside the door, ready to bring in necessary supplies and to consult. Gila Zarbiv, a midwife expert in infectious disease prevention, was inside the room “gloved and masked, with only my eyes visible,” she said. “It was hard.”
By July, 25 women with Covid-19 (“Whom we know of,” cautioned Braverman) had delivered at Hadassah, along with hundreds more with suspected infection. “Intake for those harboring or suspected of harboring the virus is separate,” said Zarbiv, “and we set up three delivery areas—for women positive for the virus, suspected of it and negative.”
With the coronavirus surging by mid-summer, Hadassah Hospital in Ein Kerem opened two rooms in the Round Building’s Covid-19 isolation unit for infected mothers. “Both rooms have been occupied since they opened,” said Rely Alon, deputy director of the division of Nursing and Health Professions.
Along with responding to pandemics and shouldering their regular workload, Hadassah midwives have created two unique programs. Come Let’s Talk, initiated by Braverman, has counseled several hundred pregnant women who experienced negative or problematic past births or sexual, physical or emotional trauma. Its interventions range from something as straightforward as noting in the file if a woman desperately wants an epidural to building a birth plan for a sexual abuse survivor.
Typically for such survivors, explained Zarbiv, “none of us touch her. There is no vaginal exam. She pushes when she feels the urge. We give her the birth experience she needs.”
The second program, created by senior midwife Kerem Tzadik, is known as Debriefing and is for women recovering from difficult births. The mother discusses what happened with a midwife who was not present at the birth. One first-time mother, for example, had not slept for weeks because the peaceful natural birth amid scented candles that she planned became a medical emergency when cord prolapse threatened to asphyxiate her emerging baby. After talking through what had happened, she could sleep again.
While the pandemic, trauma and emergencies inevitably make headlines, Hadassah’s midwives see every birth as a major event, and all have tales to tell. Meirovich recalls a woman whose labor was not progressing. “When nothing helped, I asked her: ‘What do you think is happening here?’ She burst into tears. ‘I’m so afraid,’ she sobbed, ‘afraid of not loving this baby like my other two.’ I urged her: ‘Think of somewhere you can gather strength.…Perhaps that’s from God, from your mother.’ Soon after we finished talking, she gave birth.”
She also recalls a frail 18-year-old Israeli Arab, rushed in by ambulance. “She was in advanced labor, in pain and clearly terrified,” Meirovich said of the first-time mother. “She let me listen for the baby’s heartbeat but shied away when I tried to check her dilation. In my poor Arabic, I told her I wouldn’t examine her, her baby’s heart was strong, she was almost there and doing amazingly.”
Because the laboring mother seemed overwhelmed by the delivery space, Meirovich dimmed and quieted the room, making sure to touch her only when absolutely necessary. “I watched the monitors, and she had a beautiful natural birth,” said Meirovich. “A medical student there, witnessing her first birth, cried when the baby was born.”
Wendy Elliman is a British-born science writer who has lived in Israel for more than four decades.








 Facebook
Facebook Instagram
Instagram Twitter
Twitter

Leave a Reply