Health + Medicine
Feature
Hadassah Has Israel’s Highest-Volume Cornea Clinic
Charlotte Goller has had vision problems since her early teens. By her mid-30s, she had lost almost all sight in her left eye. Its dime-sized outer covering, the cornea, had bulged outward, the distorted cone-shape no longer able to bend the incoming rays of light into the orderly patterns essential for sight.
The condition is “called keratoconus, and I was born with it,” said the Connecticut-born Goller, a 75-year-old retired clinical psychologist. In the 1980s, she underwent a full corneal transplant in her left eye from a donor cornea at Mount Sinai Hospital in New York City, and a decade later, shortly before making aliyah in 1994, she had a corneal transplant in her other eye.
Whole corneas have been successfully implanted since 1905, making it the oldest and most successful type of human tissue transplantation. But, as Goller discovered, the transplant can come with an expiration date.
“A few years back, the donor cornea in my left eye began clouding,” she said. “Soon, the eye was virtually blind again. With repeat whole corneal transplants usually rejected, I didn’t know what to do.”
Enter Goller’s sister, who happens to be Barbara Sofer, Israel director of public relations and communications for Hadassah. In 2019, Sofer introduced Goller to Dr. Itay Lavy, a senior ophthalmologist and surgeon at the Hadassah Medical Organization.
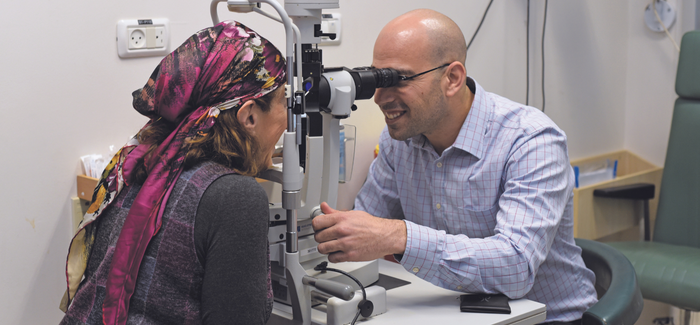
Dr. Lavy is a global expert in a cutting-edge method of partial corneal transplantation known as DMEK, Descemet’s membrane endothelial keratoplasty. His plan for Goller was to use DMEK to graft not a whole cornea, but a single microscopic layer of corneal tissue into her eye to restore her sight.
He had learned this innovative surgery during his fellowship at the Netherlands Institute for Innovative Ocular Surgery in Rotterdam with the creator of the procedure, Dutch ophthalmologist Dr. Gerrit Melles. When Dr. Lavy returned to Israel in 2017, he introduced it to Hadassah—making the medical center one of a handful of places worldwide to perform this advanced surgery.
“Hadassah has Israel’s highest-volume cornea clinic and has successfully implanted whole corneas to treat corneal trauma and disease for more than 50 years,” he said. “Now, the time limit on the implants is bringing many of these patients back with graft failure.”
In Goller’s case, as in many who need corneal transplants, “only one of the cornea’s five layers had failed, so only one needed replacing,” explained Dr. Lavy. The procedure takes about 30 minutes and is done under local anesthetic. Goller recalls being awake throughout, “feeling some pressure but no discomfort,” she said.
READ MORE:
Mayaan Hoffman: Hadassah On Call’s New Podcast Host
During the procedure, a surgeon gently dissects the cornea, separating the faulty tissue layer from the healthy ones and peeling it off. “We then inject a wisp of donor tissue,” Dr. Lavy said, “which we call a ‘megillah’ because it tends to scroll. With a virtually no-touch technique unique to Hadassah, we use air current to unscroll it and get it to the right place.”
This sounds simple until you realize that this is all taking place in the realm of the microscopic. The cornea is a half-millimeter thick at its densest, and the replacement layer a mere tenth of the thickness of a piece of paper. Not only that, but the donor cells are implanted into the cornea’s innermost layer, atop supremely sensitive cells that, if damaged, will make the patient blind.
As a guide, Hadassah’s ophthalmic surgeons use Israel’s only intraoperative optical coherence tomography (OCT), a noninvasive imaging system that works on light waves rather than radiation and allows surgeons to map and measure each of the cornea’s distinct layers in real time.
Demanding as it is, the surgery’s advantages are significant.
“It has minimal rejection rates, fast visual recovery and good visual acuity,” said Dr. Lavy. “It doesn’t touch the cornea’s surface, so there’s no astigmatism. And without sutures, there’s little incidence of infection. Better yet, one donor provides sufficient tissue for two patients.”
As with hearts and lungs, the availability of donor tissue is the bottleneck of corneal grafting worldwide. Hadassah’s response to that need was to create a cornea bank 15 years ago at HMO. Directed by Dr. Avi Solomon, Hadassah’s cornea service director and ophthalmic surgeon, the bank is run by Hadassah medical students. Sixth-year student Eden Amir has headed its three-member team for the past five years.

“We’re on call 24/7 to harvest corneas from deceased patients,” said Amir. “Medical center staff alert us to potential donors. We check their medical suitability and then approach their families. It’s hard. It needs sensitivity, focus, experience, awareness of the ethical and religious values of those involved, and a sense of when to persist and when to retreat and share the grief. I’ve had hundreds of conversations with hundreds of families. No two have ever been alike.”
He recalled going to the ICU after a Muslim father of nine children had just died. “There were dozens of sorrowing relatives there,” said Amir. “I waited and then approached two men who seemed senior. I explained, they listened and then consulted the family. One after another, they agreed to give the corneas, ‘no matter who they go to.’ ”
Once the family consents and the surgeons are informed, “we gently strip away the donor corneas in a relatively simple 30-minute procedure that leaves virtually no external trace,” said Amir. The tissue is then dispatched for immediate use or preservation.
When appropriate, the bank will bring together the family of the donor with the transplant recipient. “This closes the circle for all of them,” explained Amir, adding, “I’m uplifted by the work. I meet bereaved people who, even in their anguish, still see the other.”
Cornea bank staff say they are proud that, despite limited resources, their educational and outreach efforts in the hospital and local community have seen increased donations and a vastly shortened waiting list.
Among the some 100 recipients of cornea tissue at Hadassah last year was a 53-year-old woman originally from Odessa who had made aliyah 25 years earlier. Born with congenital cataracts clouding both eyes, she had both faulty lenses replaced with artificial ones in the former Soviet Union when she was in her teens.
These old replacement lenses “unfortunately damaged her corneas, and vision deteriorated in both her eyes,” recounted Dr. Lavy. “So she underwent whole corneal transplant in one eye, but the graft became infected and the eye lost all vision. Some years ago, now in Israel, she began losing sight in her second eye. From being fully functional, she could no longer safely make herself a cup of coffee. It was heartbreaking.”
The Hadassah team operated first on the patient’s completely blind eye, replacing the old Soviet lens and restoring vision with transplanted cornea tissue. They then gave the partially sighted eye a new, more modern artificial lens, fully restoring her sight.
Another tissue recipient at Hadassah last year was a 23-year-old Ethiopian Jew who had been in a fight in a Tel Aviv bar.
“Glass from a broken bottle damaged his right eye so severely that the hospital where he was first taken wanted to remove the eye,” said Dr. Lavy.
A naval commando officer under whom the young man had served in the Israel Defense Forces contacted Hadassah.
“He’s hotheaded and gets into trouble, but he’s a good guy,” Dr. Lavy recalled the officer saying. “He pretty much grew up on the street, and he’s come a long way. He wants to go further. Please help him keep his eye.”
In a long and complex surgery, adapting operating techniques as they went, Dr. Lavy’s team rebuilt the patient’s eye, transplanting an iris and lens as well as a cornea. Today, the young man sees well enough to drive safely.
“I always try to see the person behind the eye and tailor treatment to suit him or her,” said Dr. Lavy. “I never give up. My patients know I’ll do anything to help them. I believe their trust contributes to the surgical success.”
Dr. Lavy notes that future advances in the field may reduce demand for cornea transplants or do away with it altogether. These innovations, he hopes, will include imaging that identifies cornea disease early enough to prevent it; injection rather than surgery to implant cornea cells; corneas created on 3-D printers; healing with stem cells; and if surgery is still necessary, robotic surgeons to do precision work.
Until such advances are realized, Charlotte Goller has a plan.
“When the old transplant in my second eye wears out,” she said, looking up from one of the 100-plus books she reads each year, “I’m off to see Dr. Lavy.”
Wendy Elliman is a British-born science writer who has lived in Israel for more than four decades.










 Facebook
Facebook Instagram
Instagram Twitter
Twitter

Leave a Reply